Not the monkeypox docs thought they knew
The 47,000 cases identified worldwide have upended many of those expectations. Monkeypox patients have turned up with what looked like mosquito bites, pimples or ingrown hairs, not the large pustules usually associated with the infection.
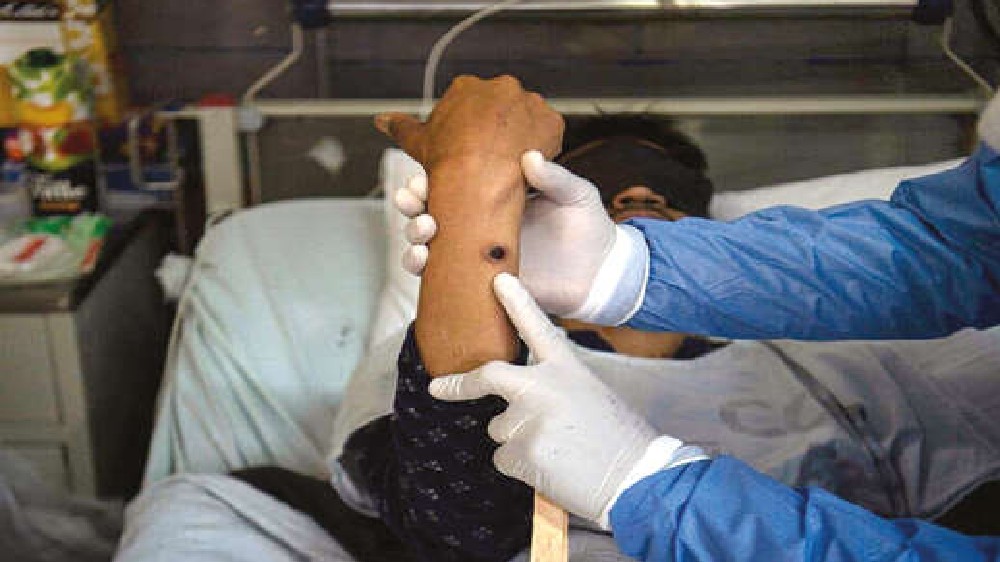
Early in the monkeypox outbreak, a man in his 20s arrived at an emergency department in Northern California, tiny blisters on his lips, hands and back. Within 12 hours, doctors diagnosed him with monkeypox. That’s where their certainty ended. The patient did not have fever, aches, weakness, pain or other symptoms typical of the disease. He did not know when or how he had become infected. He had not had sexual contact with anyone for months, he said, and had not touched — as far as he knew — anyone with pox, as the lesions are called, or other symptoms.
At the onset of the outbreak, scientists thought they knew when and how the monkeypox virus was spread, what the disease looked like and who was most vulnerable. The 47,000 cases identified worldwide have upended many of those expectations. Monkeypox patients have turned up with what looked like mosquito bites, pimples or ingrown hairs, not the large pustules usually associated with the infection. Some did not even have visible lesions but felt excruciating pain when swallowing, urinating or emptying their bowels.
Some had headaches or depression, confusion and seizures. Others had severe eye infections or inflammation of the heart muscle. At least three of the six deaths reported so far were linked to encephalitis, an inflammation of the brain. “We really are seeing a very, very wide range of presentation,” said Dr. Boghuma Titanji, an infectious disease physician at a clinic in Atlanta that serves people living with H.I.V.
Scientists now know that the monkeypox virus lurks in saliva, semen and other bodily fluids, sometimes for weeks after recovery. The virus has always been known to spread through close contact, but many researchers suspect the infection may also be transmitted through sex itself. The California patient had virus in his throat, but no respiratory symptoms, and in his rectum, but without pain or pox. The case underscores other research suggesting that the virus may be spread even by people with atypical or asymptomatic infections, said Dr. Abraar Karan, who diagnosed the patient and published a recent case report. In another study, also published this month, anal swabs of 200 men without symptoms turned up 13 who were positive for monkeypox. Only two of them later developed symptoms.
“It’s no longer correct to say it can’t be transmitted asymptomatically,” said Dr. Chloe Orkin, an infectious disease physician at Queen Mary University of London. “I think that it means that our working model of how it’s spread is incorrect.” Early in the outbreak, the C.D.C. said that “people who do not have monkeypox symptoms cannot spread the virus to others.” The agency changed that phrasing on July 29 to say that “scientists are still researching” the possibility of asymptomatic transmission.
In a statement to The New York Times, an agency spokeswoman acknowledged recent evidence that asymptomatic cases were possible but said that it was still uncertain whether people without symptoms could spread the virus and that more research was needed.
When the first few dozen cases of monkeypox emerged in Europe, spreading of the virus through sexual contact and genital lesions came as a surprise to many scientists. But it shouldn’t have. Nigerian researchers reported a similar pattern in 2017, when they documented 228 cases, many of them young men with genital ulcers. (The patients identified as heterosexual in a subsequent study, but Nigeria criminalises same-sex behavior.) Those cases were the first reported in Nigeria in 40 years, and the World Health Organization helped the country “mount the local response, with the goal to control spread,” said Fadela Chaib, a spokeswoman for the organization.
Visit news.dtnext.in to explore our interactive epaper!
Download the DT Next app for more exciting features!
Click here for iOS
Click here for Android



